Reimbursement
Telehealth reimbursement is an extremely important topic and ever-changing. It is important to understand that there is a difference in “coverage” versus “reimbursement” for telehealth visits.
While an insurance policy may state that a telehealth visit is “covered,” it is important to note the amount for that visit may not be the same payment coverage as a face-to-face encounter.
Insurance carriers are beginning to expand their telehealth options to their clients, but the patient and provider need to be aware of which services are covered and at what rate.
CMS is the main driver of telehealth payment models. The private insurance sector will often follow guidance from Federal programs such as CMS. The trend of private insurances reimbursing for telehealth was increasing prior to the pandemic and they are expected to continue to increase. Currently, Medicare has increased their coverage to include synchronous video, remote patient monitoring (RPM), and some additional inter-provider telehealth codes. It is important to reiterate that “coverage” does not equal payment parity. Parity laws are defined as reimbursement for telehealth services at the same rate of comparable in-person service. Some codes, such as RPM codes, are based on a per patient, per month fee. You can find a complete list of CMS coverage codes and policies at the following link: CMS Medicare Learning Network Telehealth Policy Coverage.
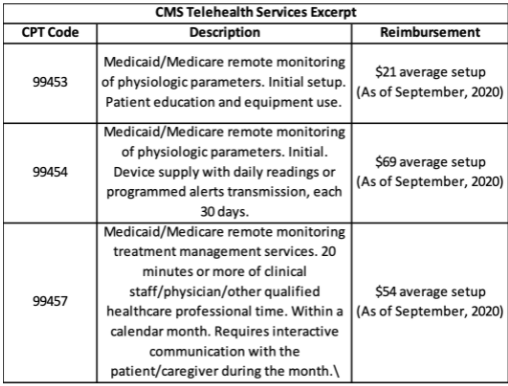
While CMS is a Federal governing body, it is up to each state to determine what their particular State Medicaid benefits will cover. The list of current NC Medicaid covered services and codes can be found on the Medicaid site. The current Medicare Fee Schedule can be found here on the website.
An important note for North Carolina practitioners is understanding telehealth originating and distant site coverage. An originating site is the location where a beneficiary receives telehealth services. The beneficiary must be located at the originating site. The distant site is the location where the provider is located and can receive payment for covered services (subject to state law). It is important for providers to check with individual payors about which telehealth services are covered and if there are telehealth site restrictions.
While noting the specifics around site policies, it is important to keep up to date with the changes in place of service payment policies through Medicare and Medicaid. All of the newest policies can be found here, FQHC and RHC specific details are located at the bottom of this link.
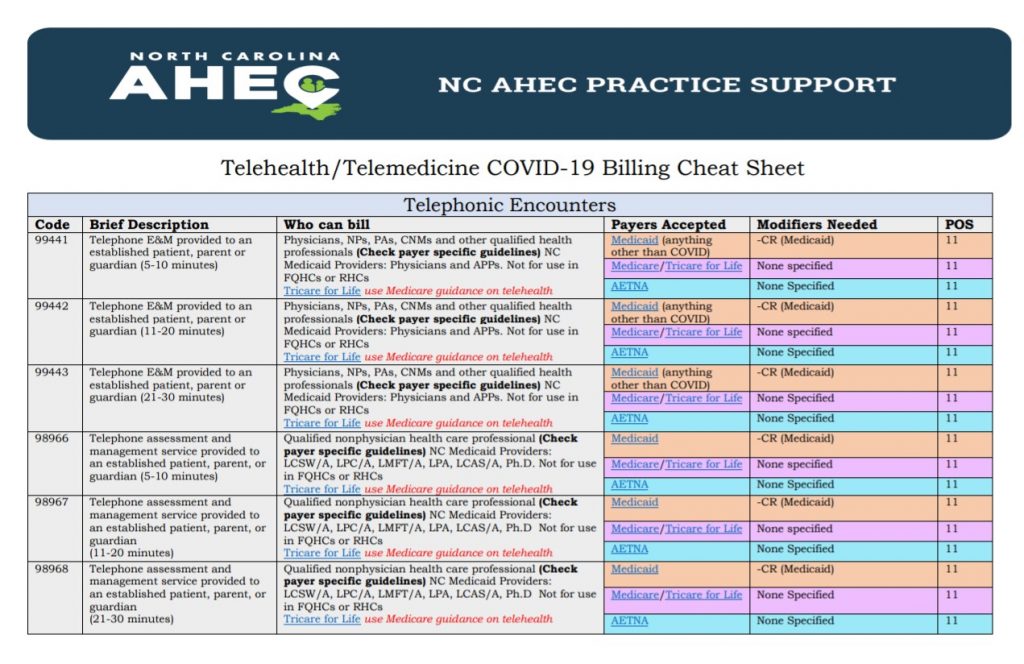
Telehealth reimbursement took a significant step forward in response to the COVID-19 Pandemic. Both Federal and State governments increased telehealth funding opportunities so that providers could care for their patients and increase access to health care through telehealth. These changes went into effect as of March 2020; however, the long-term evolution and policy practices are still unclear. There are many resources on the NC Medicaid, AHEC and CCNC websites with state specific billing and coding tips like the example listed below.